Neisseria and Moraxella
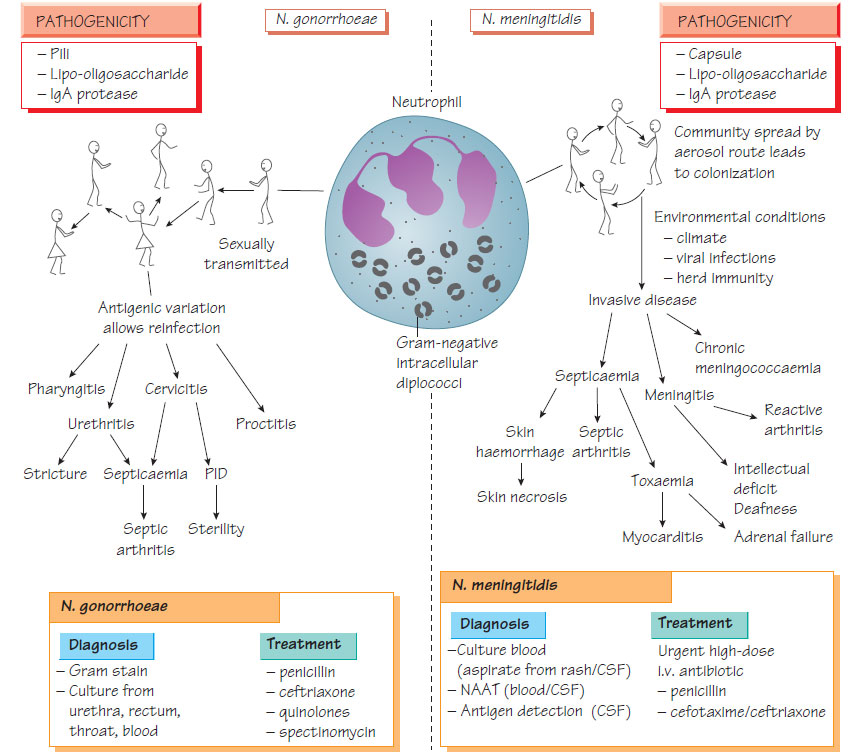
Neisseria gonorrhoeaeInfection with Neisseria gonorrhoeae, a Gram-negative diplococcus, is most common in individuals between 15 and 35 years of age. It is almost exclusively spread by sexual contact.
Pathogenesis
The organism adheres to the genitourinary epithelium via pili, then invades the epithelial layer and provokes a local acute inflammatory response. Variation in the proteins of the pili means that infection does not provide protection against re-infection, therefore infections with another strain of different antigenic structure are possible.
- Acute painful urethritis and urethral discharge.
- Female infection (cervicitis) is often asymptomatic or associated with vaginal discharge.
- Pelvic inflammatory disease (PID) may develop (see Urinary and genital infections).
- Pharyngeal infection causes sore throat.
- Rectal infection causes a purulent proctitis.
- Infection can be complicated by bacteraemia, septic or reactive arthritis of the large joints, or pustular rashes.
- Late complications include female infertility and male urethral stricture.
Diagnosis
The optimal diagnostic technique is a nucleic acid amplification test (NAAT) on urethral or vaginal swabs, or urine. Positive samples are then cultured for susceptibility testing.
Treatment must be given before susceptibility results are available and is based on the known susceptibility patterns found at the clinic, as emergence of resistance is a problem. Ceftriaxone, spectinomycin or fluoroquinolones may be used. Gonorrhoea can be prevented by avoiding sexual contact with individuals at high risk and using effective barrier contraception. Contacts of infected individuals should be traced and treated. At present vaccine development is precluded by the antigenic variation that occurs within the pili.
Neisseria meningitidis
Epidemiology
Carriage of Neisseria meningitidis (meningococcus) is common; actual disease only develops in a few individuals. Infection is most common in the winter, with epidemics occurring every 10-12 years. In Africa, severe epidemics of group A infection occur in the 'meningitis belt' where the incidence can rise to 1000 cases per 100 000 each year. Most invasive infections are caused by serogroups A, B or C. Group B infection is now the commonest, as the incidence of group C infection has reduced in communities where vaccination has become routine. A group A vaccination programme is being implemented in Africa.
- An antiphagocytic polysaccharide capsule that allows survival in the bloodstream.
- Lipo-oligosaccharide activates complement and stimulates cytokine release, which leads to shock and disseminated intravascular coagulation (DIC).
- The organism hijacks the β2-adrenoreceptor to cross the brain vascular endothelium.
- Meningococci cross mucosal epithelium by endocytosis. Meningococcal meningitis is characterized by fever, neck stiffness and reduced consciousness. The petechial rash, a sign of septicaemia, may be present without other signs of meningitis. Septic or reactive arthritis may develop.
Diagnosis and Treatment
The diagnosis is usually made clinically and confirmed by culture of blood, aspirate from the rash and CSF. Rapid antigen detection or NAAT on CSF and blood are sensitive and reliable. Infection is life-threatening and rapidly progressive; treatment should not await laboratory confirmation or hospitalization. Intravenous benzylpenicillin (intramuscular in the community setting) is the antibiotic of choice, but there have been reports of meningococci with reduced susceptibility in other countries and cefotaxime is an alternative. Treatment does not eradicate carriage so the patient should be given 'prophylaxis' following recovery.
- A protein-conjugated serogroup C vaccine is more than 90% efficient and has vastly reduced the incidence where it has been introduced.
- An effective vaccine against serogroup B is not available, although a vaccine based on membrane proteins specific for epidemic strains has shown promise.
- Close contacts of patients with meningococcal meningitis should be given 'prophylaxis' with rifampicin or ciprofloxacin.
Moraxella catarrhalis
This Gram-negative coccobacillus is usually a commensal of the upper respiratory tract. It is associated with otitis media, sinusitis and lower respiratory tract infection in children or patients with chronic pulmonary disease. It usually produces β-lactamase.