Serology, Part 2–Indirect Serologic Testing
Using Antigen-Antibody Reactions in the Laboratory to Indirectly Diagnose Disease, By Detecting Antibodies in a Person’s Serum Produced against a Disease AntigenIndirect serologic testing is the procedure whereby antibodies in a person’s serum being made by that individual against an antigen associated with a particular disease are detected using a known antigen.
The Concept and General Procedure for Indirect Serologic Testing
The concept and general procedure for this type of serological testing are as follows:
- Concept. This type of testing is based on the fact that antibodies are only
produced in response to a specific antigen. In other words, a person will
not be producing antibodies against a disease antigen unless that antigen
is in the body stimulating antibody production.
- General Procedure. A sample of the patient’s serum (the liquid portion of the blood after clotting and containing antibodies against the disease antigen if the person has or has had the disease) is mixed with the known antigen for that suspected disease. One then looks for an antigen-antibody reaction. Examples of serologic tests to diagnose disease by the detection of antibodies in the patient’s serum include the various serological tests for syphilis or STS (such as the RPR, VDRL, and FTA-ABS tests), tests for infectious mononucleosis, tests for the human immunodeficiency virus (HIV), tests for systemic lupus erythematosus, and tests for variety of other viral infections.
Qualitative and Quantitative Serologic Tests
Indirect serologic tests may be qualitative or quantitative. A qualitative test only detects the presence or absence of specific antibodies in the patient’s serum and is often used for screening purposes. A quantitative test shows the titer or amount of that antibody in the serum. Titer indicates how far you can dilute the patient’s serum and still have it contain enough antibodies to produce a detectable antigen-antibody reaction. In other words, the more antibodies being produced by the body, the more you can dilute the person’s serum and still see a reaction. Quantitative serological tests are often used to follow the progress of a disease by looking for a rise and subsequent drop in antibody titer.
Detection of Antigen-antibody Reactions in the Laboratory
Antigen-antibody reactions may be detected in the laboratory by a variety of techniques. Some of the commonly used techniques are briefly described below:
- Agglutination. Antibodies in the patient’s serum cause the known particulate antigens or cells to clump or agglutinate. Molecular-sized known antigens can be attached to larger, insoluble particles such as latex particles, red blood cells, or charcoal particles in order to observe agglutination with the naked eye.
- Precipitation. The patient’s serum is mixed with soluble known antigen and a cloudy precipitate forms at the zone of optimum antigen-antibody proportion.
- Complement-fixation. The patient’s serum is mixed with the known antigen and a complement is added. Sheep red blood cells and hemolysins (antibodies that lyse the sheep red blood cells in the presence of free complement) are then added. If the complement is tied up in the first antigen-antibody reaction, it will not be available for the sheep red blood cell-hemolysin reaction and there will be no hemolysis. A negative test would result in hemolysis.
- Enzyme immunoassay (EIA). The patient’s serum is placed in a tube or well coated with the corresponding known antigen and becomes trapped on the walls of the tube. Enzyme-labeled anti-human gamma globulin or anti- HGG (antibodies made in another animal against the Fc portion of human antibody and to which an enzyme has been chemically attached), is then passed through the tube, where it combines with the trapped antibodies from the patient’s serum. Substrate for the enzyme is then added and the amount of antibody-antigen complex formed is proportional to the amount of enzyme-substrate reaction, as indicated by a color change.
- Radioactive binding techniques. The patient’s serum is passed through a tube coated with the corresponding known antigen and becomes trapped on the walls of the tube. Radioisotope-labeled anti-human gamma globulin or anti-HGG (antibodies made in another animal against the Fc portion of human antibody and to which a radioactive isotope has been chemically attached), is then passed through the tube, where it combines with the trapped antibodies from the patient’s serum. The amount of antibodyantigen complex formed is proportional to the degree of radioactivity measured.
- Fluorescent antibody technique. The patient’s serum is mixed with known antigen fixed to a slide. Fluorescent anti-human gamma globulin or anti- HGG (antibodies made against the Fc portion of human antibody and to which a fluorescent dye has been chemically attached) is then added. It combines with the antibodies from the patient’s serum bound to the antigen on the slide, causing the antigen to fluoresce when viewed with a fluorescent microscope.
Examples of Indirect Serologic Tests to Detect Antibodies in the Patient’s Serum
The RPR Test for Syphilis
Syphilis is a sexually transmitted disease caused by the spirochete Treponema pallidum. The RPR (Rapid Plasma Reagin) Card® test is a presumptive serologic screening test for syphilis. The serum of a person with syphilis contains a nonspecific antilipid antibody (traditionally termed reagin), which is not found in normal serum. The exact nature of the antilipid (reagin) antibody is not known, but it is thought that a syphilis infection instigates the breakdown of the patient’s own tissue cells. Fatty substances that are released then combine with protein from Treponema pallidum to form an antigen that stimulates the body to produce antibodies against both the body’s tissue lipids (nonspecific or nontreponemal), as well as the T. pallidum protein (specific or treponemal). The RPR Card® test detects the nonspecific antilipid antibody and is referred to as a nontreponemal test for syphilis.
It must be remembered that tests for the presence of these nonspecific antilipid antibodies are meant as a presumptive screening test for syphilis. Similar reagin-like antibodies may also be present as a result of other diseases such as malaria, leprosy, infectious mononucleosis, systemic lupus erythematosus, viral pneumonia, measles, and collagen diseases, and may produce biologic false-positive results (BFP). Confirming tests should be made for the presence of specific antibodies against the T. pallidum itself. The confirming test for syphilis is the FTA-ABS test. Any serologic test for syphilis is referred to commonly as an STS (Serological Test for Syphilis).
The known RPR antigen consists of cardiolipin, lecithin, and cholesterol bound to charcoal particles in order to make the reaction visible to the naked eye. If the patient has syphilis, the antilipid antibodies in his or her serum will cross-react with the known RPR lipid antigens, producing a visible clumping of the charcoal particles.
We will do a quantitative RPR Card® test in the lab. Keep in mind that a quantitative test allows one to determine the titer or amount of a certain antibody in the serum. In this test, a constant amount of RPR antigen is added to dilutions of the patient’s serum. The most dilute sample of the patient’s serum still containing enough antibodies to produce a visible antigen-antibody reaction is reported as the titer.
Serologic Tests for Infectious Mononucleosis
During the course of infectious mononucleosis, caused by the Epstein-Barr virus (EBV), the body produces nonspecific heterophile antibodies that are not found in normal serum. As it turns out, these heterophile antibodies will also cause horse or sheep erythrocytes (red blood cells) to agglutinate.
The infectious mononucleosis serologic test demonstrated here is a rapid qualitative test for infectious mononucleosis that uses specially treated horse erythrocytes (acting as the “known antigen”) that are highly specific for ononucleosis heterophile antibodies. Agglutination of erythrocytes after adding the patient’s serum indicates a positive test. Quantitative tests may be done to determine the titer of heterophile antibodies and follow the progress of the disease.
Serologic Tests for Systemic Lupus Erythematosus (SLE)
Systemic lupus erythematosus, or SLE, is a systemic autoimmune disease. Immune complexes become deposited between the dermis and the epidermis, and in joints, blood vessels, glomeruli of the kidneys, and the central nervous system. It is 4 times more common in women than in men. In SLE, autoantibodies are made against components of DNA. This test is specific for the serum antideoxyribonucleoprotein antibodies associated with SLE. The known antigen is deoxyribonucleoprotein adsorbed to latex particles to make the reaction more visible to the eye. This is a qualitative test used to screen for the presence of the disease and monitor its course.
Detecting Antibody Using the Indirect Fluorescent Antibody Technique: The FTA-ABS Test for Syphilis
The indirect fluorescent antibody technique involves 3 different reagents:
- The patient’s serum (containing antibodies against the disease antigen if the disease is present)
- Known antigen for the suspected disease
- Fluorescent anti-human gamma globulin antibodies (antibodies made in another animal against the Fc portion of human antibodies by injecting an animal with human serum). A fluorescent dye is then chemically attached to the anti-human gamma globulin (anti-HGG) antibodies.
The FTA-ABS test (Fluorescent Treponemal Antibody Absorption Test) for syphilis is an example of an indirect fluorescent antibody procedure. This is a confirming test for syphilis since it tests specifically for antibodies in the patient’s serum made in response to the syphilis spirochete, Treponema pallidum.
In this test, killed T. pallidum, (the known antigen), is fixed on a slide. The patient’s serum is added to the slide. If the patient has syphilis, antibodies against the T. pallidum will react with the antigen on the slide. The slide is then washed to remove any antibodies not bound to the spirochete.
To make this reaction visible, a second animal-derived antibody made against human antibodies and labeled with a fluorescent dye (fluorescent antihuman gamma globulin) is added. These fluorescent anti-HGG antibodies react with the patient’s antibodies, which have reacted with the T. pallidum on the slide. The slide is washed to remove any unbound fluorescent anti-HGG antibodies and observed with a fluorescent microscope. If the spirochetes glow or fluoresce, the patient has made antibodies against T. pallidum and has syphilis.
The EIA and Western Blot Serologic Tests for Antibodies Against the Human Immunodeficiency Virus (HIV)
In the case of the current HIV antibody tests, the patient’s serum is mixed with various HIV antigens produced by recombinant DNA technology. If the person is seropositive (has repeated positive antigen-antibody tests), then HIV must be in that person’s body stimulating antibody production. In other words, the person must be infected with HIV. The 2 most common tests currently used to detect antibodies against HIV are the enzyme immunoassay, or EIA (also known as the enzyme-linked immunosorbant assay, or ELISA) and the Western blot, or WB. A person is considered seropositive for HIV infection only after an EIA screening test is repeatedly reactive and another test, such as the WB, has been performed to confirm the results.
The EIA is less expensive, faster, and technically less complicated than the WB and is the procedure initially done as a screening test for HIV infection. The various EIA tests produce a spectrophotometric reading of the amount of antibody binding to known HIV antigens.
The EIA test kit contains plastic wells to which various HIV antigens have been adsorbed. The patient’s serum is added to the wells and any antibodies present in the serum against HIV antigens will bind to the corresponding antigens in the wells. The wells are then washed to remove all antibodies in the serum other than those bound to HIV antigens. Enzyme-linked anti-human gamma globulin (anti-HGG) antibodies are then added to the wells. These antibodies, made in another animal against the Fc portion of human antibodies by injecting the animal with human serum, have an enzyme chemically attached. They react with the human antibodies bound to the known HIV antigens.
The wells are then washed to remove any anti-HGG that has not bound to serum antibodies. A substrate specific for the enzyme is then added and the resulting enzyme-substrate reaction causes a color change in the wells. If there are no antibodies against HIV in the patient’s serum, there will be nothing for the enzyme-linked anti-HGG to bind to, and it will be washed from the wells. When the substrate is added, there will be no enzyme present in the wells to produce a color change.
If the initial EIA is reactive, it is automatically repeated to reduce the possibility that technical laboratory error caused the reactive result. If the EIA is still reactive, it is then confirmed by the Western blot (WB) test.
The WB is the test most commonly used as a confirming test if the EIA is repeatedly positive. The WB is technically more complex to perform and interpret, is more time-consuming, and is more expensive than the EIAs.
With the WB, the various protein and glycoprotein antigens from HIV are separated according to their molecular weight by gel electrophoresis (a procedure that separates charged proteins in a gel by applying an electric field). Once separated, the various HIV antigens are transferred to a nitrocellulose strip. The patient’s serum is then incubated with the strip and any HIV antibodies that are present will bind to the corresponding known HIV antigens on the strip. Enzyme-linked anti-human gamma globulin (anti-HGG) antibodies are then added to the strip. These antibodies, made in another animal against the Fc portion of human antibodies by injecting the animal with human serum, have an enzyme chemically attached. They react with the human antibodies bound to the known HIV antigens. The strip is then washed to remove any anti-HGG that has not bound to serum antibodies. A substrate specifically for the enzyme is then added and the resulting enzyme-substrate reaction causes a color change on the strip. If there are no antibodies against HIV in the patient’s serum, there will be nothing for the enzyme-linked anti-HGG to bind to, and it will be washed from the strip. When the substrate is added, there will be no enzyme present on the strip to produce a color change.
It should be mentioned that all serologic tests are capable of producing occasional false-positive and false-negative results. The most common cause of a false-negative HIV antibody test is when a person has been only recently infected with HIV and his or her body has not yet made sufficient quantities of antibodies to give a visible positive serologic test. It generally takes between 2 weeks and 3 months after a person is initially infected with HIV to convert to a positive HIV antibody test.
Procedure
The RPR® Card Test for Syphilis
- Label 6 test tubes as follows: 1:1, 1:2, 1:4, 1:8, 1:16, and 1:32.
- Using a 1.0-mL pipette, add 0.5 mL of 0.9% saline solution into tubes 1:2, 1:4, 1:8, 1:16, and 1:32.
- Add 0.5 mL of the patient’s serum to the 1:1 tube (undiluted serum).
- Add another 0.5 mL of serum to the saline in the 1:2 tube and mix. Remove 0.5 mL from the 1:2 tube, add it to the 1:4 tube, and mix. Remove 0.5 mL from the 1:4 tube, add to the 1:8 tube, and mix. Remove 0.5 mL from the 1:8 tube, add to the 1:16 tube, and mix. Remove 0.5 mL from the 1:16 tube, add to the 1:32 tube, and mix. Remove 0.5 mL from the 1:32 tube and discard.
- Using the capillary pipettes provided with the kit, add a drop of each serum dilution to separate circles of the RPR card. Spread the serum over the entire inner surface of the circle with the tip of the pipette, using a new pipette for each serum dilution.
- Using the RPR antigen dispenser, add a drop of known RPR antigen to each circle. Do not let the needle of the dispenser touch the serum. Using disposable stirrers, mix the known RPR antigen with the serum in each circle.
- Place the slide on a shaker and rotate for a maximum of 4 minutes.
- Read the results as follows:
- A definite clumping of the charcoal particles is reported as reactive (R).
- No clumping is reported as nonreactive (N).
The greatest serum dilution that produces a reactive result is the titer. For example, if the dilutions turned out as follows, the titer would be reported as 1:4 or 4 dils.
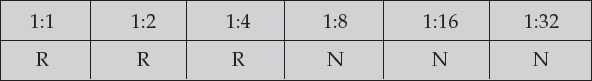 |
The Serologic Tests for Infectious Mononucleosis
- Place 1 drop of each of the patient’s serum in circles on the test slide.
- Add 1 drop of treated horse erythrocytes (the known antigen) to each circle and mix with disposable applicator sticks.
- Rock the card gently for 1 minute, then leave undisturbed for 1 minute, and observe for agglutination of the red blood cells. Agglutination indicates the presence of heterophile antibodies.
The Serologic Tests for Systemic Lupus Erythematosus (SLE)
- Add 1 drop of each of the patient’s serum to separate circles on the test slide.
- Add one drop of the latex-deoxyribonucleoprotein reagent (the known antigen, deoxyribonucleoprotein adsorbed to latex particles) to each serum sample and mix with disposable applicator sticks.
- Rock the slide gently for 1 minute and observe for agglutination. Agglutination indicates the presence of antinuclear antibodies associated with SLE.
The FTA-ABS Test for Syphilis (Indirect Fluorescent Antibody Technique)
Observe the 35-mm slide of a positive FTA-ABS test.
The EIA and WB Tests for HIV Antibodies
Observe the illustrations of the EIA and the WB tests for antibodies against HIV.
Results
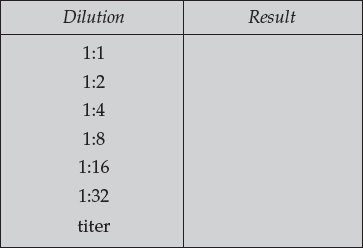
RPR Card® Test for Syphilis (Quantitative)
- Detects nontreponemal antilipid antibodies (reagin).
- Record your results in the table.
 |
||
|
MONO-Test for Infectious Mononucleosis (Qualitative)
- Detects heterophile antibodies.
- Draw the results of both positive and negative tests.
 |
| Figure 56 Infectious mononucleosis test slide. |
+ = agglutination of RBCs – = no agglutination of RBCs |
Serologic Test for SLE (Qualitative)
- Detects anti-deoxyribonucleoprotein antibodies.
- Draw the results of both positive and negative tests.
 |
| Figure 57 SLE test slide.. |
+ = agglutination – = no agglutination |
FTA-ABS Test for Syphilis (Confirming)
- Detects antibodies against Treponema pallidum.
- Draw the results of a positive FTA-ABS test.
Performance Objectives
Discussion
- Explain the principle and general procedure behind indirect serologic testing.
- Explain the difference between a qualitative serological test and a quantitative serological test.
- Define titer.
- Name which disease the RPR and the FTA-ABS procedures test for. Indicate which of these is a presumptive test, which is a confirming test, and why?
- Describe the significance of nontreponemal antilipid (reagin) antibodies in
serological testing. - Describe the significance of heterophile antibodies in serological testing.
- Explain the significance of anti-deoxyribonucleoprotein antibodies in serological testing.
- Briefly describe the indirect fluorescent antibody technique.
- Briefly describe the EIA test for HIV antibodies and the significance of a positive HIV antibody test.
- Name the most common reason for a false-negative HIV antibody test.
Results
- Interpret the results of the following serological tests:
- Serologic test for infectious mononucleosis
- Serologic test for SLE
- FTA-ABS test
- Determine the titer of a quantitative RPR Card® test.




