Pathogenic mycobacteria
Mycobacteria possess a lipid-rich cell wall that retains some dyes, resisting decolourization with acid (hence they are known as acid-fast). There are more than 50 species; although most are environmental organisms that rarely cause human infection.Mycobacterium tuberculosis
Epidemiology and pathogenesis
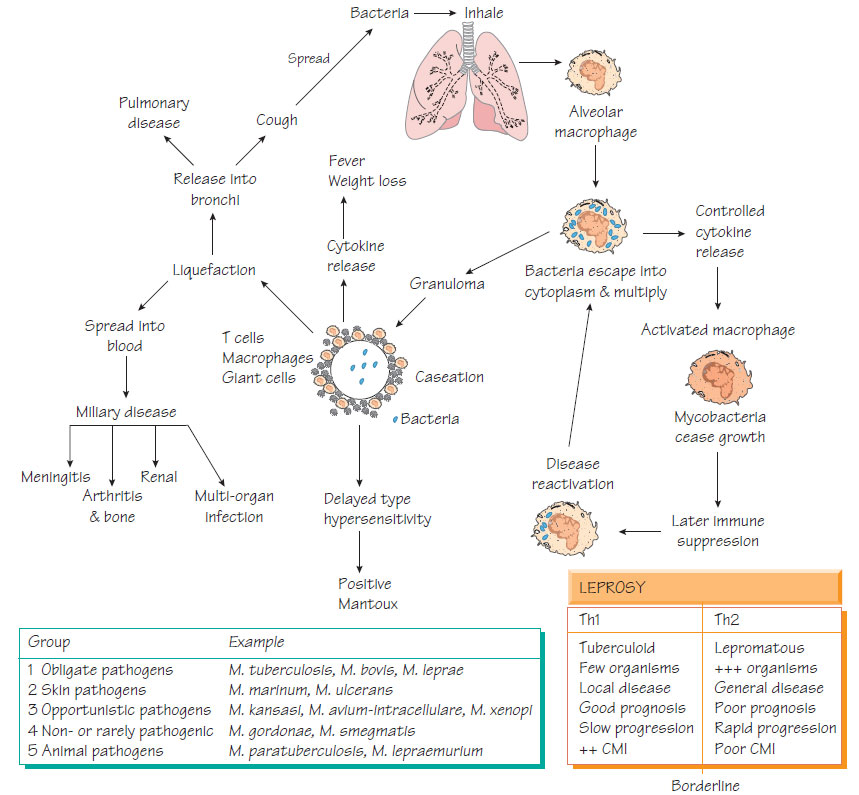
Tuberculosis is spread from person to person by the airborne route. In childhood, the lung is the first site of infection and most infections resolve with local scarring (the primary complex). In about 5% the infection is not controlled and it spreads from the primary focus throughout the body (miliary spread). This may resolve spontaneously or develop into other localized infections (e.g. meningitis, osteomyelitis). Disease may emerge if immunity wanes or in later life (10% lifetime risk). Immunity depends on effective T-cell function so if compromised, individuals are more likely to develop symptomatic disease.
Mycobacterium tuberculosis is ingested by macrophages but escapes from the phagolysosome to multiply in the cytoplasm. The intense immune response causes local tissue destruction (cavitation in the lung) and cytokine-mediated systemic effects (fever and weight loss). Many antigens have been identified as possible virulence determinants, including lipoarabinomannan (stimulates cytokines) and superoxide dismutase (promotes intramacrophage survival).
Mycobacterium tuberculosis may affect every organ of the body mimicking both inflammatory and malignant diseases.
- Pulmonary: chronic cough, haemoptysis, fever and weight loss, or recurrent bacterial pneumonia. If untreated, it follows a chronic, deteriorating course.
- Meningitis: fever and deteriorating level of consciousness.
- Renal: signs of local infection, fever and weight loss, complicated by ureteric fibrosis and hydronephrosis.
- Bone: the lumbosacral spine is a common site of infection. Complicated by vertebral collapse and nerve compression. Pus may spread under the psoas sheath to appear in the groin (psoas abscess).
- Joints: infects large joints causing destructive arthritis.
- Abdominal: mesenteric lymphadenopathy and chronic peritonitis may present as fever, weight loss, ascites and intestinal malabsorption.
- Miliary disease: may occur without evidence of active lung infection.
A wide range of specimens can be examined, using a variety of techniques.
- Direct staining with Ziehl-Neelsen's method or auramine.
- Culture on lipid-rich (egg-containing) medium with malachite green (L�wenstein-Jensen or L-J medium) to suppress other organisms.
- Automated growth detection, which can speed isolation.
- Susceptibility is usually tested in automated systems (e.g. Mycobacterial Growth Indicator Test [MGIT]).
- Nucleic acid amplification tests (NAATs) that include detection of drug resistance mutations allow rapid identification of patients with multidrug resistance TB (MDRTB) so they can be isolated and appropriately treated.
- Typing by identification of the number of copies of 23 repetitive DNA elements.
- Immunity is determined by measuring the ?-interferon response to specific antigens (Interferon Gamma Release Assay [IGRA]).
The standard regimen for pulmonary infection is rifampicin and isoniazid for 6 months, with ethambutol and pyrazinamide for the first 2 months. Regimens for other sites are similar, taking into account drug penetration (e.g. into CSF). There is a rising trend of MDRTB. Features that predispose a patient to this include:
- previous incomplete treatment;
- being a known contact of an MDR patient;
- residence in a country where MDRTB is common;
- failure to respond to an adequate regimen.
Treatment of MDRTB is complex, requiring a combination of second-line agents, such as aminoglycosides, fluoroquinolones, ethionamide or cycloserine, guided by susceptibility tests.
Vaccination with attenuated bacille Calmette-Gu�rin (BCG) strain may protect against miliary spread, but trials in some countries have shown no benefit. Patients at high risk of developing tuberculosis may be given prophylaxis with isoniazid and rifampicin.
Mycobacterium leprae attacks peripheral nerves, causing anaesthesia. Digital destruction and deformity follow, leaving the patient severely disabled. The end result of infection depends on the individual immune response, forming a spectrum from 'tuberculoid' dominated by a Th1 response, through 'borderline', to 'lepromatous' dominated by a Th2 response. Patients with tuberculoid disease have a stronger immune response, more localized disease and fewer bacteria. With lepromatous disease there is poor cellmediated immunity (CMI) and generalized disease (leonine facies, depigmentation and anaesthesia).
Diagnosis is by Ziehl-Neelsen's stain of a split-skin smear and histological examination of a skin biopsy. Treatment with rifampicin, dapsone and clofazimine rapidly renders the patient non-infectious, but cannot alter nerve damage and deformity, which must be managed by remedial surgery.
Mycobacterium marinum causes a chronic granulomatous infection of the skin and is acquired from rivers, poorly maintained swimming pools or fish tanks. It is characterized by encrusted pustular lesions. M. ulcerans infection is associated with farming in Africa and Australia. The lower limb is usually affected with a papular lesion, which ulcerates and may destroy underlying tissue including bone.